Achieve the Highest Positive Payment Adjustment
It’s 2017 and that marks the first reporting year of the MACRA program. The most common MACRA questions to hit my inbox this year are:
- “What can we do to avoid a payment adjustment?”, and
- “What can I do to receive the highest incentive payment?”
Here is an overview of the MIPS point scale and tips on achieving positive payment adjustments.
Tip: Leverage the CMS “Pick Your Pace” option. There are several ways to reach your incentive payment goals and avoid negative adjustments.
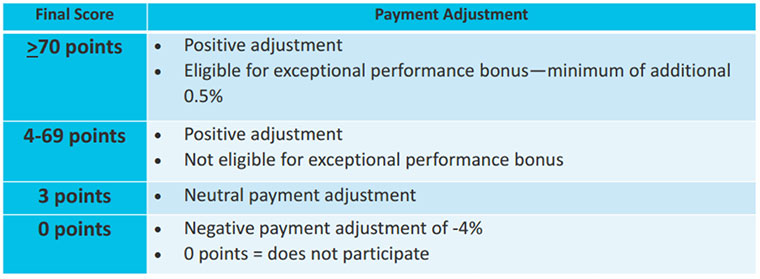
Tip: Understand the MIPS Point Scale. The table posted below shows how the 100-point MIPS scale works. The program and scale are outlined on a webinar and in materials sponsored by CMS and the Medicare Learning Network (PDF).

MIPS Point Scale Overview
Points are calculated based on practice performance in four key categories:
- Quality
- Cost
- Improvement activities, and
- Advancing care information
The better your performance in each category, the higher your overall rating, leading to improved incentive payments. Check the table to see how points are accumulated toward higher payments.
CMS will continue to offer resources to help you understand this transition and achieve optimal incentive payments. Check the CMS site to learn more and check for more posts about MACRA and Healthcare IT on our blog.
MACRA and MIPS may seem confusing programs to many practices – especially those that may not have the resources or time to explore these new rules in detail. Rest assured that eMedApps is committed to assisting providers through all phases of the MACRA and MIPS transition. Our healthcare IT experts are ready to help, just contact us for more information.
